Health and Well Being
- Asthma
- Depression
- Heart Disease
- Immunization
- Influenza
- Substance Use Disorder
- Stroke
Asthma
 Control your asthma and breathe with ease. Asthma is a chronic condition that occurs when the bronchial tubes (the lungs’ main air passages) become inflamed. The bronchial wall muscles tighten, producing excess mucus and causing the airways to narrow. This constriction causes conditions ranging from minor wheezing to severely labored breathing.
Control your asthma and breathe with ease. Asthma is a chronic condition that occurs when the bronchial tubes (the lungs’ main air passages) become inflamed. The bronchial wall muscles tighten, producing excess mucus and causing the airways to narrow. This constriction causes conditions ranging from minor wheezing to severely labored breathing.
Though asthma is not typically considered a life-threatening lung disease, each year, nearly 500,000 Americans are hospitalized for asthma-related conditions and more than 4,200 die. Recognizing warning signs and treating symptoms early can help control your asthma and prevent it from getting worse.
You can help better manage asthma by limiting your exposure to environmental factors that aggravate the condition. Second-hand smoke is just as—if not more—devastating to people with asthma, but affects them slowly. Tobacco smoke contains nearly 400 toxic substances and carcinogens that irritate air passages but do not necessarily cause coughing or wheezing during exposure. It is particularly detrimental for children with asthma when an adult smokes in the home.
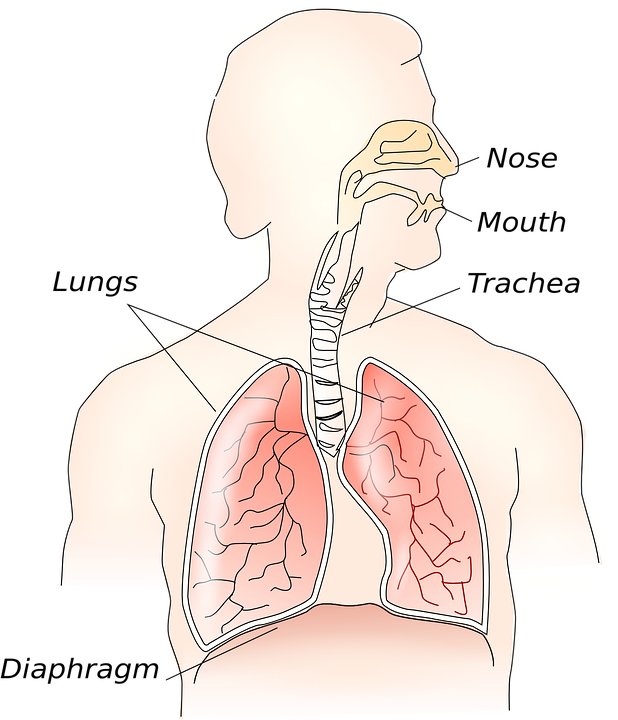 See your doctor if you think you have asthma. Signs include wheezing, labored breathing, chest pain or tightness, and coughing without any other symptoms.
See your doctor if you think you have asthma. Signs include wheezing, labored breathing, chest pain or tightness, and coughing without any other symptoms.
If you’ve been diagnosed with asthma, ask your doctor how to manage your condition. Together, you and your doctor can develop a plan to help control your symptoms and prevent attacks. If your prescribed medication does not alleviate your symptoms, contact your doctor immediately.
Asthma should not limit your activities or cause depression. You can still live an active life if your asthma is controlled by carefully following your doctor’s treatment plan. It’s also important to avoid certain triggers, such as smoke, dust, or mold. Once you understand how to manage your condition, you can breathe with greater ease.
Depression
 Clinical depression, the most common mental health problem, affects nearly 20 million Americans each year. And that number is probably significantly higher because, nationally, fewer than half of those suffering from clinical depression seek treatment.
Clinical depression, the most common mental health problem, affects nearly 20 million Americans each year. And that number is probably significantly higher because, nationally, fewer than half of those suffering from clinical depression seek treatment.
What is depression?
Depression is a medical illness, and like many other illnesses, it can be managed effectively with the appropriate treatment. It is more than being sad or discouraged, which are normal feelings that typically pass in a few days. Depression is a persistent condition that can make daily activities difficult, affecting your physical health and well-being as well as those around you. Its severity can range from a mild, depressive mood that is experienced almost daily to persistently intense feelings of sadness, hopelessness, or significant loss of interest and pleasure.
What causes depression?
The exact causes of depression are not fully understood. What we do know is that depression is a medical condition, not a character or personality flaw. The most common conditions that can accompany depression are:
• Chemical imbalances in the brain.
• Certain medical illnesses.
• Certain medications.
• Alcohol and/or drug use.
• Stressful life events.
Who’s at risk?
 Though anyone can suffer from depression, individuals with other medical conditions are at greater risk. Depression affects as many as one-third of all patients with chronic medical conditions, such as diabetes, cancer, or heart disease.
Though anyone can suffer from depression, individuals with other medical conditions are at greater risk. Depression affects as many as one-third of all patients with chronic medical conditions, such as diabetes, cancer, or heart disease.
How can you recognize symptoms of clinical depression? Look for these signs:
• Persistent sad, anxious, or “empty” mood.
• Sleeping too much or too little, and waking up in the middle of the night or early morning.
• Reduced appetite and weight loss, or increased appetite and weight gain.
• Loss of pleasure and interest in activities once enjoyed.
• Restlessness or irritability.
• Persistent physical symptoms such as chronic pain or digestive disorders that do not respond to treatment.
• Difficulty concentrating, remembering, or making decisions.
• Fatigue or loss of energy.
• Feeling guilty, hopeless, or worthless.
• Thoughts of suicide or death.
If you have five or more of these symptoms for two weeks or more, you could have clinical depression and should see your doctor or a qualified mental health professional for help.
Again, remember that clinical depression is treatable. Treatment usually includes antidepressant medication, psychotherapy, or a combination of the two.
Of course, treatment depends on the severity of the condition. In some cases of mild to moderate depression, increasing your physical activity, taking up a new hobby, or joining a social group or club may help alleviate some of your depression symptoms.
And remember, there’s no shame in seeking help.
Heart Disease
Not having enough good cholesterol (HDL) and having too much bad cholesterol (LDL) can put you at risk for heart disease, which can lead to a heart attack or stroke. There are some risk factors you can’t do anything about, such as age or family history. But there are things you can do to help improve your cholesterol levels:
• Know your risk. High cholesterol is often called a “silent disease” because there are no major symptoms. Major risk factors include diabetes, premature coronary heart disease, high blood pressure, and cigarette smoking. Men age 45 and older and women age 55 and over are also at high risk.
• Get tested. If you’re at high risk or over the age of 20, talk to your doctor about a cholesterol screening.
• Set a goal. The ideal LDL for a high-risk patient is < 100 mg/dL. Work with your doctor to decide on an appropriate cholesterol goal and come up with a plan to manage your levels.
• Lead a healthy lifestyle. Improve your diet by avoiding foods high in cholesterol and saturated fat, increase exercise, maintain a healthy weight, avoid smoking, and take your medication correctly.
• Practice good oral hygiene and see a dentist regularly. Patients with poor oral hygiene may have up to twice the risk of having a heart attack.
 It is estimated that 25 percent of people who should be taking statins, or cholesterol-lowering drugs, do not take them. Studies have shown 20 percent to 60 percent lower LDL cholesterol levels in people who take statins. Speak to your physician about the possibility of taking a generic drug — they cost much less and are often just as effective.
It is estimated that 25 percent of people who should be taking statins, or cholesterol-lowering drugs, do not take them. Studies have shown 20 percent to 60 percent lower LDL cholesterol levels in people who take statins. Speak to your physician about the possibility of taking a generic drug — they cost much less and are often just as effective.
Blood Pressure
When blood pressure is high, your heart must work harder to move blood through your body. Over time, this can lead to serious health problems such as heart disease, heart attack, stroke, blindness, or kidney disease.
High blood pressure, or hypertension, often has few symptoms. One in three adults has it, but many don’t know it. The only way to know if your blood pressure is in a healthy range (120/80 for most people) is to have it checked regularly by your doctor.
Hypertension is caused by a number of factors. Some, like genetics, cannot be controlled. However, there are many risk factors you can change to keep your blood pressure at a healthy level.
• Maintain a healthy diet. Avoid foods high in sodium, fat, and cholesterol. Eat more fruits, vegetables, whole grains, and low-fat dairy products.
• Increase your physical activity. Exercise for at least 30 minutes on most days. Exercise can even come in the form of routine chores, like yard work or walking your dog.
• Maintain a healthy weight. Losing excess weight can reduce unnecessary stress on the heart, which can help alleviate many heart conditions.
• Avoid alcohol and smoking. More than one to two drinks per day can increase fat levels in the blood. Smoking cigarettes constricts and damages blood vessels.
• Reduce your stress. A strong emotional reaction to a stressful event is a common trigger for heart attacks. Learn to stay calm during stressful times.
If changing your lifestyle habits doesn’t reduce your blood pressure, your doctor may prescribe medication. Don’t hesitate to talk to your doctor if you have questions or experience adverse side effects; many options are available and they may be able to prescribe another medication.
Know your blood pressure numbers. This could save your life.
• High blood pressure (hypertension): 140/90 or above
• Borderline high blood pressure (pre-hypertension): 120/80 to 139/89
• Healthy blood pressure: Below 120/80
CDC immunization schedules can be found at: https://www.cdc.gov/vaccines/schedules/index.html

School Immunizations:
Children entering kindergarten, or seventh grade in Utah are required to receive certain immunizations before school begins. This protects the child, and the whole community against potentially harmful diseases that can be life-threatening, especially in children and babies. Family Healthcare offers no-charge childhood vaccinations to families without health care insurance or with financial need. No child is ever turned away from receiving their immunizations. This is a proven way to ensure children grow and stay healthy.
School Entry Immunization Requirements in Utah |
|
Entering Kindergarten |
Entering seventh grade |
|
|
For more information on school entry requirements and immunizations, check out the Utah Department of Health’s guidance at www.immunize-utah.org |
|
Preschool Immunizations:
Children attending a preschool program, including a licensed daycare center, nursery, childcare facility, family home care, or Head Start Program are required to be immunized appropriately for the age of the child. Preschoolers should receive all the doses of each vaccine for their age group, and according to current immunization schedules as published by the Utah Department of Health.
COVID-19 Info
Follow this link to see helpful information for Family Healthcare patients pertaining to COVID-19 vaccines and vaccination sites.
Flu Shots
To see the locations offering flu shots for Family Healthcare patients, please click this link.

Influenza or ‘Flu’
Influenza, commonly called ‘Flu’ is a contagious respiratory illness caused by influenza viruses that infect the nose, throat, and sometimes the lungs. It can cause mild to severe illness, and at times can lead to death.
The best ways to prevent flu are:
- Annual flu vaccine
- Washing hands
- Avoid touching face before washing hands
- Maintaining a healthy immune system as much as possible by getting enough rest, regular exercise, and following a healthy diet
Flu Symptoms:
- fever* or feeling feverish/chills
- cough
- sore throat
- runny or stuffy nose
- muscle or body aches
- headaches
- fatigue (tiredness)
- some people may have vomiting and diarrhea, though this is more common in children than adults.
- *not everyone with flu experiences a fever.
Treating the flu is best done by staying home and resting, drinking plenty of fluids, and visiting your healthcare provider if symptoms do not improve or worsen.

Call Family Healthcare at:
- St. George & Hurricane – 435-986-2565
- Cedar City – 435-865-1387
Substance Use Disorder
The terms “substance abuse” and “substance dependence” have been replaced with “substance use disorder.” Substance use disorder is now the medical term for addiction. Previously, abuse was a mild form of addiction, and dependence was a moderate or severe form of addiction.
According to the Center for Disease Control, one in 14 Americans reports experiencing a substance use disorder. There is not one single driving factor that leads to addiction. Some people may use drugs to help cope with stress, trauma, or to help with mental health issues. Some may even develop opioid use disorder after misusing opioids they are prescribed by doctors. In any case, using drugs over time makes it easier to become addicted.
A substance use disorder occurs when the recurrent use of alcohol and/or drugs causes clinically significant impairment, including health problems, disability, and failure to meet major responsibilities at work, school, or home.
Addiction is a treatable disease
Addiction is a disease, not a character flaw. People suffering from substance use disorders have trouble controlling substance use even though they know these substances are harmful.
Overcoming a substance use disorder is not as simple as resisting the temptation through willpower alone. Recovery may involve medication to help with cravings and withdrawal as well as different forms of therapy. It may even require checking into a rehabilitation facility. Recovery can be challenging, but it is possible.
Opioids
Prescription opioids cause 36 deaths a month in Utah. Utah ranked 4th in the US for drug poisoning death.
Death from prescription opioid outnumbers deaths by all other illicit drugs combined.
In Utah, Opioid deaths outnumbered deaths by all other illicit drugs combined.
In 2016, the CDC reported opioid prescribing rates per 100 persons. Utah’s prescribing rate was 70.4, while the overall rate in the nation was 66.5.
Both Washington and Iron Counties reported higher prescription rates in 2016, at rates of 89 and nearly 104, respectively.
In 2017, Utah saw a slight decrease in the number of prescription opioid deaths, however, the number of heroin deaths that have increased during the same time period. Many people who have had their opioid prescriptions discontinued seek and buy street drugs such as Heroin or Fentanyl.
At Family Healthcare clinics, we practice an integrated health system when treating people with prescription opioid abuse. We screen patients who come thought us through family and loved ones intervention and those who are sent to us through the court system, or those who have finally reached a decision to get help.
The patient meets with a team who assess the willingness and readiness of the patients. Our Medicine Assisted Treatment or MAT team is comprised of a medical provider, a nurse practitioner, behavior health specialist, Registered Nurse, and medical assistants. The patient is evaluated and a treatment plan is formulated.
The solution lies in integrated care, the systematic coordination of general and behavioral healthcare. Integrating mental health, substance abuse, and primary care services produces the best outcomes and proves the most effective approach to caring for people with multiple healthcare needs.
It is the policy of Family Health Care to assure appropriate clinical management of patients with opioid addiction to control their opioid abuse and addiction. Our goal is to relieve unnecessary pain and suffering and improve our patient’s quality of life, while doing our best to ensure safety for our patients as well as our community.
Medication Assisted Treatment (MAT)
The use of FDA approved medications, in combination with counseling and behavioral therapies for the treatment of substance use disorders. The prescription medication helps to normalize brain chemistry, block the euphoric effect of substances, relieve physiological cravings, and normalize body functions. The goal of MAT is full recovery, including the ability to live a self-directed life. This treatment approach has been shown to:
- Improve patient survival
- Increase patient retention in treatment
- Increase patient ability to gain and maintain employment
- Improve birth outcomes among women who have substance use disorders and are pregnant
- Decrease illicit substance use and other criminal activities among people with substance use disorders
Prescriptions
Receive your prescriptions at 40% to 60% off the usual price when they are ordered by your Family Healthcare provider and filled at any of the following pharmacies:
- Hurricane Family Pharmacy
- Cedar Drug
Additional Treatment Options
- Twelve-step facilitation therapy is an individual active engagement strategy designed to encourage people to accept drug addiction as a chronic, progressive disease and prepare them to begin a 12-step mutual support program.6
- Outpatient counseling can help people understand addiction, their triggers, and their reasons for using drugs. This form of treatment can be done at a doctor’s office or via telehealth appointment.
- Inpatient rehabilitation at a full-time facility provides a supportive environment to help people recover without distractions or temptations.
Signs of overdose
Recognizing the signs of opioid overdose can save a life. Here are some things to look for:
- Small, constricted “pinpoint pupils”
- Falling asleep or losing consciousness
- Slow, weak, or no breathing
- Choking or gurgling sounds
- Limp body
- Cold and/or clammy skin
- Discolored skin (especially in lips and nails)
What to do if you think someone is overdosing
It may be hard to tell whether a person is high or experiencing an overdose. If you aren’t sure, treat it like an overdose—you could save a life.
- Call 911 Immediately.*
- Administer naloxone, if available. **
- Try to keep the person awake and breathing.
- Lay the person on their side to prevent choking.
- Stay with the person until emergency assistance arrives.
*Most states have laws that may protect a person who is overdosing or the person who called for help from legal trouble.
Naloxone
Naloxone is a life-saving medication that can be used in the event of a known or suspected opioid overdose. This medication is available for free at our Family Healthcare Riverside Pharmacy and in many other pharmacies around the country.
For more information about Substance Use Disorders, please visit the Utah Department of Human Services – Substance Use and Mental Health at https://dsamh.utah.gov/substance-use-disorder
Stroke
 A stroke occurs when the blood supply to part of your brain is interrupted or reduced, depriving brain tissue of oxygen and nutrients. Within minutes, brain cells begin to die.
A stroke occurs when the blood supply to part of your brain is interrupted or reduced, depriving brain tissue of oxygen and nutrients. Within minutes, brain cells begin to die.
A stroke is a medical emergency. Prompt treatment is crucial. Early action can minimize brain damage and potential complications.
The good news is that strokes can be treated and prevented, and many fewer Americans die of stroke now than in the past.
Symptoms
Watch for these signs and symptoms if you think you or someone else may be having a stroke. Pay attention to when the signs and symptoms begin. The length of time they have been present can affect your treatment options:
- Trouble with speaking and understanding. You may experience confusion. You may slur your words or have difficulty understanding speech.
- Paralysis or numbness of the face, arm or leg. You may develop sudden numbness, weakness or paralysis in your face, arm or leg. This often happens just on one side of your body. Try to raise both your arms over your head at the same time. If one arm begins to fall, you may be having a stroke. Also, one side of your mouth may droop when you try to smile.
- Trouble with seeing in one or both eyes. You may suddenly have blurred or blackened vision in one or both eyes,or you may see double.
- Headache. A sudden, severe headache, which may be accompanied by vomiting, dizziness or altered consciousness, may indicate you’re having a stroke.
- Trouble with walking. You may stumble or experience sudden dizziness, loss of balance or loss of coordination.
When to see a doctor
Seek immediate medical attention if you notice any signs or symptoms of a stroke, even if they seem to fluctuate or disappear. Think “FAST” and do the following:
- Face. Ask the person to smile. Does one side of the face droop?
- Arms. Ask the person to raise both arms. Does one arm drift downward? Or is one arm unable to rise up?
- Speech. Ask the person to repeat a simple phrase. Is his or her speech slurred or strange?
- Time. If you observe any of these signs, call 911 immediately.
Call 911 or your local emergency number right away. Don’t wait to see if symptoms stop. Every minute counts. The longer a stroke goes untreated, the greater the potential for brain damage and disability.
If you’re with someone you suspect is having a stroke, watch the person carefully while waiting for emergency assistance.

We continue to evolve Family Healthcare according to the model of the Patient Centered Medical Home (PCMH) which puts patients at the center of the healthcare system, and provides primary care that is “accessible, affordable, continuous, comprehensive, family centered, coordinated, compassionate, and culturally effective.”
We are looking for various roles across our care teams and administration. If you want to help others and make lives better through compassionate quality healthcare service delivery, then we’d love to hear from you!
HOW DID WE DO?
PLEASE LEAVE A REVIEW









